Keratoconus
What is Keratoconus?
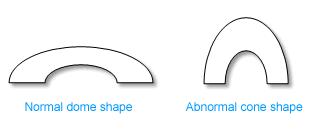
Keratoconus is a progressive eye disease that causes a thinning of the cornea, the clear front surface of the eye. The cornea, which is the clear, dome-shaped front surface of the eye. In individuals with keratoconus, the cornea gradually thins and bulges outward, adopting a more conical shape instead of its normal rounded shape. This irregularity in the corneal shape leads to visual distortions and refractive errors.
Keratoconus is usually a bilateral condition but one eye may progress faster than the other. Familial occurrence has been noted although most cases show no definitive inheritance pattern.
The cause of keratoconus is not fully understood, but it is believed to be caused by a combination of genetic, environmental, and hormonal factors. It often begins during teenage years or early adulthood and may progress over several years before stabilizing.
Keratoconus Treatment with personalEYES
In the past, patients with keratoconus would have been told that they were not suitable for refractive surgery (LASIK). Today there are a number of possible options available.
Usually, the first step in keratoconus treatment is to correct the refractive error with glasses or hard contact lenses. This will help you to achieve adequate vision. As keratoconus progresses, the quality of your vision will deteriorate and contact lenses or glasses may no longer be satisfactory.
A Toric Implantable Contact Lens (built-in astigmatism) is an option that can be used in those with mild keratoconus as long as the cornea is stable and good vision can be obtained with glasses. Corneas can be stabilised by Collagen Cross-Linking.
Many of our patients require a corneal transplant. However, kera ring prescription inserts and CAIRS are other options to consider.
Cornea Cross Linking
Corneal cross-linking is a medical procedure that is used to treat keratoconus, as well as other corneal conditions. The aim of this procedure is to strengthen the cornea by creating additional cross-links between the collagen fibers, which increases its stability and halts the progression of the disease.
Studies have shown that corneal cross-linking is effective in reducing the progression of keratoconus. Additionally, it has been found to reduce corneal steepness, which can help improve the patient's vision. The procedure has also been shown to have a low risk of complications, making it a safe and viable option for treating certain corneal conditions.
Overall, corneal cross-linking is a promising treatment option for those who suffer from keratoconus or other corneal conditions. It can help improve the stability of the cornea and halt the progression of the disease, potentially improving the patient's vision and quality of life.
Kera Rings
Kera rings, also known as corneal ring segments or intracorneal ring segments, are small, crescent-shaped devices that are surgically implanted into the cornea to treat certain vision problems, including keratoconus. These rings are made of a biocompatible material and are designed to alter the shape of the cornea, improving its curvature and visual acuity.
Kera rings help to reshape the cornea, improving visual acuity and reducing the irregular astigmatism associated with conditions like keratoconus. There are other similar types of corneal ring segments available, such as Intacs, which are also used to treat corneal irregularities like keratoconus.
Corneal Allogenic Intrastromal Ring Segments (CAIRS)
Corneal allogenic intrastromal ring segments (CAIRS) refer to the use of donor corneal tissue for the placement of intrastromal ring segments to treat certain corneal conditions, including keratoconus. Allogenic refers to the fact that the donor tissue comes from another individual.
Corneal allogenic intrastromal ring segments aim to improve corneal shape and visual acuity by altering the corneal curvature. They provide support and help stabilize the cornea in conditions such as keratoconus.
The CAIRS procedure is generally covered by health funds.
Stages of Keratoconus Treatment
- Eyeglasses in the early stages.
- Rigid contact lenses when eyeglasses do not work.
- CXL – Corneal Collagen Cross-Linking with Riboflavin – increases the strength of the cornea to prevent progress.
- Kera rings (Intracorneal rings) – when there is intolerance to contact lenses and when the condition continues to progress.
- CAIRS (Corneal Adaptive Image Refractive System) - combines two treatment methods to address both the strengthening of the cornea and the correction of corneal irregularities.
- Corneal transplant in advanced stages – either a partial thickness (Deep Anterior Lamellar or DALK) or full thickness (Penetrating or PK).
We at personalEYES may be able to explore various procedures to help you become independent from contact lenses &/or glasses.